PI’s: Chunhui Xu & Nael McCarty
β-blockers are unsuccessful in eliminating stress-induced ventricular arrhythmias in approximately 25% of patients with catecholaminergic polymorphic ventricular tachycardia (CPVT). Induced pluripotent stem cell-derived cardiomyocytes (iPSC-CMs) generated from these patients have potential for investigating the phenomenon, but it remains unknown whether they can recapitulate patient-specific drug responses to β-blockers. This study assessed whether the inadequacy of β-blocker therapy in an individual can be observed in vitro using patient-derived CPVT iPSC-CMs. A CPVT patient harboring a novel mutation in the type 2 cardiac ryanodine receptor (RyR2) was identified whose persistent ventricular arrhythmias during β-blockade with nadolol were abolished during flecainide treatment. iPSC-CMs generated from this patient and two control individuals expressed comparable levels of excitation-contraction genes, but assessment of the sarcoplasmic reticulum Ca2+ leak and load relationship revealed intracellular Ca2+ homeostasis was altered in CPVT iPSC-CMs.
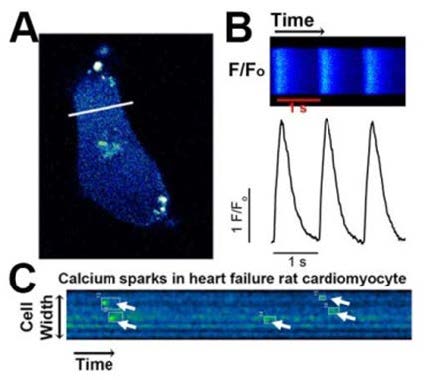
β-adrenergic stimulation potentiated spontaneous Ca2+ waves and unduly frequent, large, and prolonged Ca2+ sparks in CPVT compared to control iPSC-CMs, validating the disease phenotype. Pursuant to the patient’s in vivo responses, nadolol treatment during β-adrenergic stimulation achieved negligible reduction of Ca2+ wave frequency and failed to rescue Ca2+ spark defects in CPVT iPSC-CMs. In contrast, flecainide reduced both frequency and amplitude of Ca2+ waves and restored the frequency, width, and duration of Ca2+ sparks to baseline levels. By recapitulating a CPVT patient’s improved response to flecainide compared to β-blocker therapy in vitro, these data provide new evidence that iPSC-CMs can capture basic components of patient-specific drug responses.


